Enrollment in Health First Colorado (Colorado’s Medicaid Program) and Child Health Plan Plus (CHP+) continued to increase throughout Q3, July through September of 2020. Enrollment in Health First Colorado’s non-disability programs including Modified Adjusted Gross Income (MAGI) and CHP+ increased by a combined total of 54,714 individuals, or 4.7 percent of the enrolled population.
Specifically, in Q3 2020, the total number of adults, pregnant adults, and children enrolled in Health First Colorado MAGI programs increased by 59,717 individuals, or 5.5 percent. However, the total number of children and pregnant adults enrolled in CHP+ decreased by 5,003 individuals, or 6.6 percent. This decrease could be because many of the children in CHP+ likely transitioned to Health First Colorado over the last quarter.
Figure 1.
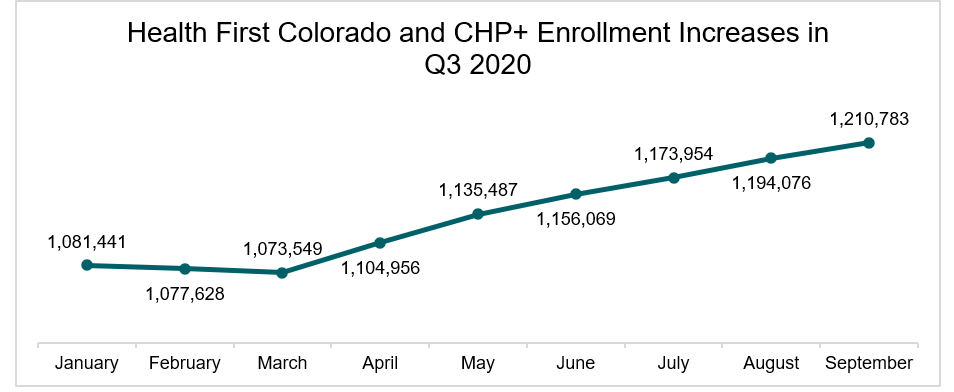
Figure 1 shows an increase in Health First Colorado and CHP+ enrollment during 2020. Additional details and graphs on Q3 enrollment are available in CKF’s 2020 Q3 Health First Colorado and CHP+ Enrollment Analysis.
There are a few reasons for the increase:
Continuous Eligibility Requirement: The Continuous Eligibility (CE) requirement of the Families First Coronavirus Response Act, states that no Medicaid member enrolled on or after March 18, 2020, can be disenrolled from benefits unless the member voluntarily terminates their benefits, moves out of state, becomes incarcerated, or dies. Therefore, with very few people disenrolling, new enrollments show a more visible net increase. This requirement will continue until the end of the month when the Public Health Emergency expires, which is currently January 2021.
Unemployment: Despite the overall decrease in unemployment during Q3, from 7.4 percent in July to 6.4 percent in September, many Coloradans who lost their jobs since March 2020 likely became eligible for Health First Colorado or CHP+ benefits for the first time.[1]
Challenges in In-Person Application Assistance: Some organizations that offered remote application assistance for Health First Colorado and CHP+ returned to offering in-person application assistance during Q3. and allowed more Coloradans to successfully enroll in health coverage. Many sites, especially those certified by Connect for Health Colorado, focused on remote-only assistance due to guidance from Connect for Health Colorado which enabled them to do so. For example, application assistance sites supporting Health First Colorado and CHP+ applications were challenged to meet the state’s requirements for a ‘wet signature’ while offering enrollment assistance remotely. Covering Kids and Families (CKF) recognizes the hardship this causes on application assistance sites and potential applicants. CKF continues to advocate for guidance from The Colorado Department of Health Care Policy and Financing on remote enrollment assistance so that sites that are not certified by Connect for Health Colorado can operate remotely as well.
Looking to the Future:
We anticipate a continued increase in enrollment followed by a steep decrease when the CE requirement ends at the end of the month when the PHE ends, currently set for January 31, 2021. Please reach out to Shoshi Preuss with any comments or questions on this article or the changes in enrollment.
[1] U.S. Bureau of Labor Statistics, Economy at a Glance: Colorado, https://www.bls.gov/eag/eag.co.htm
Leave A Comment